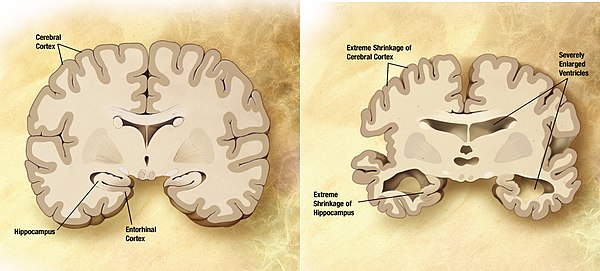
Amyloid Plaque, Vitamin C, and Alzheimer’s Disease
We are now well aware of the importance of the gut microbiome, but did you know we also have a brain microbiome? Like with the gut, the brain’s microbiome contains a mix of “good” and “bad bacteria”.
This recent discovery led Harvard researchers, Dr. Rudolph Tanzi and Robert D. Moir, PhD, to initiate a study designed to map the microbiome that exists in our brains.
“The Brain Microbiome Project”, is a follow up on their earlier research, in which they discovered the amyloid plaque found in brains of Alzheimer’s patients, may not be the cause of this disease. They found that the amyloid beta protein (the main component of amyloid plaque) is an “antimicrobial peptide”, which is used by the brain’s immune system to protect itself from infection. (Brain Microbiome Project Article)
Amyloid Plaque is Trying to Protect Us
With this new study they hope to confirm the thesis that amyloid plaque is a result of the brain attempting to protect itself from invasive material. And they hope to define exactly what the brain is defending against.
According to their initial research, the amyloid-beta proteins are protecting (rather than damaging) brain cells, by surrounding viruses, bacteria, and fungi, isolating and segregating the offending pathogens so they can not harm the brain.
Once the amyloid beta plaque has entrapped the microbes, it generates a burst of oxygen radicals which destroys the pathogens. The plaque then remains in the brain sealing in any microbes that may have survived the killing process.
Unfortunately, when these amyloid plaque clumps get prolific, they cause inflammation, and the formation of neurotoxic tangles, these in turn lead to the death of nerve cells, ultimately resulting in Alzheimer’s disease.
“What we now have is convincing data from animal models that amyloid-beta functions in humans as an antimicrobial peptide.” (Source)
Here I will mention my three blogs on The Real Cause of Alzheimer’s Disease, which may be worth reading for those of you who have yet to do so. These blogs are based on a study that examined brain tissue from 18 subjects who died with fully developed AD. According to this study, “100% of the AD patients analyzed thus far by our laboratory present fungal cells and fungal material in brain sections.” This material further supports the hypothesis that amyloid plaque is not the cause of Alzheimer’s.
The Role of Vitamin C in Alzheimer’s
Meanwhile, other researchers are examining a different theory of Alzheimer’s disease, one that begins by looking at vitamin C. This research is based on two principles: the brain stores more vitamin C than any of our other organs; and levels of vitamin C are lower in Alzheimer’s patients than in healthy people. In fact, even with adequate dietary intake of vitamin C, Alzheimer’s patients have lower levels of vitamin C in their blood plasma, and cerebrospinal fluid. And, people who take vitamin C supplements show reduced risk for developing Alzheimer’s.
Furthermore, laboratory animals bred to develop Alzheimer’s show improvement in symptoms when supplemented with vitamin C. (These rodents are genetically engineered so they cannot produce vitamin C, making them more akin to humans, for the purposes of this study.) When dosing these experimental animals repeatedly with high amounts of vitamin C, beta amyloid plaque levels in their brains was reduced by 40 (hippocampus) to 58% (cortex). (Study)
The researchers have a theory as to why vitamin C is so important for preventing Alzheimer’s.
How Vitamin C Protects
One of the first things that happens during the development of Alzheimer’s disease is blood leaks from weak capillaries in the brain, into surrounding tissues. This process occurs years before amyloid plaque builds up, leading to the destruction of brain cells. The researchers point out that vitamin C keeps capillaries strong, so they are less likely to break and leak blood into brain tissues.
At this point I will add that vitamin C works in tandem with bioflavonoids to maintain and strengthen veins and capillaries. Therefore, ensure that you are taking bioflavonoids along with your vitamin C. Given that regular vitamin C users are at a reduced risk of getting Alzheimer’s, it is suggested that those concerned follow a protocol for vitamin C that facilitates the best risk reduction. Vitamin C is water soluble, and thus rapidly moves through the body, and is not stored. The ideal way to get the protective benefits from vitamin C is through repeated dosing, taking 500 to 1000 mg, every 4 to 6 hours.
I will also mention our Liposomal Vitamin C product, which, while it does not contain bioflavonoids, does have the ability to get the vitamin C through the blood brain barrier, offering more protection than conventional vitamin C. As well, liposomal vitamin C stays in the blood longer than even buffered vitamin C, so is a good choice for those who do not have the time, or inclination, to take vitamin C frequently throughout the day. (Liposomal Vitamin C)
Other Vitamin C Mechanisms
Aside from vitamin C’s ability to strengthen blood vessels, there are perhaps a couple of other mechanisms by which it might also aid in preventing Alzheimer’s. One is vitamin C’s ability to elevate glutathione production in the body: every time we take 500 mg (or more) of vitamin C we get a boost in glutathione production.
“Glutathione has been implicated as a critical factor in the cognitive impairment of Alzheimer’s disease as well as non-Alzheimer’s cognitive impairment owing to its ability to help the body cope with oxidative stress.” (Source)
The second mechanism may simply be that vitamin C is antimicrobial. If indeed the function of amyloid plaque is to protect the rest of the brain from pathogenic microbes, then having vitamin C mop up some of those bad bacteria, may also contribute to preventing Alzheimer’s. (Study)
Conclusion
Given this new data, the scientists involved believe a new approach to testing is required. They suggest that measuring levels of beta amyloid plaque should be discontinued, and replaced with testing levels of vitamin C in blood and cerebrospinal fluid levels, this approach being a better indicator of risk for Alzheimer’s disease. (Source)